“One Ascension” Journey to Define a Unified Image Across Hundreds of Its Hospitals
In 1999, Ascension Health was formed when the Daughters of Charity united with the Sisters of St. Joseph health system. Restructured as Ascension in 2012, the company furthered its mission of serving those who are struggling the most and delivering compassionate care to lead healthcare transformation in the United States. Over the years, various other hospitals and clinics joined the system.
Served as one of the largest national healthcare systems in the United States, Ascension includes more than 160,000 associates and 40,000 aligned providers. It operates more than 2,600 sites of care, including 139 hospitals and more than 40 senior living facilities in 19 states and the District of Columbia.
To achieve those impressive numbers, the company has to be committed to its mission with a team of experienced and talented leaders who have made the right decisions along the way. Key drivers toward this success are the efforts to reorganize the structure, to build a unified brand, to keep up with the digital innovation, and to find out an effective revenue cycle management solution.
Empower the Youth Movement by Restructuring
At the beginning of 2019, the industry has seen a decline in inpatient admissions over time as more care is delivered outside the walls of a traditional hospital. In the meantime, outpatient services represented 53% of the overall patient revenue, illustrating the shift from inpatient to outpatient. Additionally, non-traditional vendors are threatening to shake up the status quo and siphoning patients away from traditional players like Ascension by providing care faster and cheaper at retail locations.
For those reasons, the reorganization came as Ascension moves in a new strategic direction, shifting its focus from inpatient care on its hospital campuses to improving the overall health of its communities through quick and easy access points. In doing so, the company announced it was eliminating the two-division structure and that three top executives would leave, including Patricia Maryland, executive vice president of Ascension and president and CEO of Ascension Healthcare at that time.

To Maryland, the restructuring would help the company become agile and reactive to the current health care needs. By flattening the company, reorganization allowed the healthcare system to create a direction and an alignment between its strategy, annual operations, and the ability to be able to execute. This new flatter organization made the system more efficient and empower its new, young leaders to have more authority and accountability to help lead through the market changes.
“What we’re doing is now empowering those market leaders to drive strategy and action in the shape in their local market. Why go through another person to do that? We are giving them more authority, more capability,” Maryland said. “We believe they’re prepared to do that and many of them have gone through our leadership academy program and have learned how to be a key leader in driving change within their market and be effective in terms of doing that.”
Advancing Mission Is One of the Top Priorities
According to president and CEO Joseph Impicciche, his first priority is advancing the company’s mission to deliver compassionate, personalized care to all with special attention to persons living in poverty and those most vulnerable. The mission calls Ascension’s teams to be advocates for a compassionate society through their actions and their words.
“Our mission is foundational to our work to transform healthcare,” said Impicciche. “One of my top priorities has also been to advance Ascension’s efforts to transform healthcare through innovation across the continuum of care. To accomplish this, I have worked closely with our senior leadership team to guide all elements of our health ministry’s operations through our advanced strategic direction and Mission-inspired Transformation.”
The company has announced the Mission-inspired Transformation model as a way to guide efforts to reimagine new ways of working to support its mission and focus to deliver personalized care to all individuals and communities served. Since launching this model, the teams have been able to make important decisions faster and find a renewed sense of connection to the mission.
As Impicciche informed, the initiative is three-fold: evolve Ascension’s operating model to create more integrated, empowered teams that foster greater alignment and accountability; advance an organizational culture defined by a participatory community of high-functioning teams, compassionate caregivers, and servant leaders; and adopt collaborative, multidisciplinary teams to implement innovative solutions using design thinking and agile ways of working.

With this restructured operating model and flattened organizational approach, Ascension has been able to tap into the unique skills and contributions of both longtime and next-generation leaders with varied backgrounds and talents. As Impicciche believed, “Despite the challenges and rapid pace of change, one thing that continues to stand the test of time is our mission.”
“Our collaborative teams bring together multidisciplinary groups of associates and leaders to envision and implement transformational solutions using design thinking and new ways of working,” Impicciche said. He seems to be very excited about the system’s associates and their commitment to the shared mission, which leads us to the next point.
From a Shared Mission to a Shared Brand
As patients become more and more empowered, they have a greater influence on health care choices and view them similarly to other brand choices. Because of that, Ascension decided to rebrand to evolve from being a holding company of separate health systems into an operating company to increase its brand awareness. The system’s goal is to make it clearer and easier for patients to know which hospitals are part of the Ascension brand so they can easily navigate the healthcare delivery system.
“The adoption of a consistent identity across our systems of care fosters collaboration and ultimately ensures our patients receive the right care in the right setting at the right time through a truly integrated national system,” said the former CEO of Ascension Anthony R. Tersigni.
This undertaking became known as the “One Ascension” journey and it became one of the largest such initiatives among health care organizations. Since then, Ascension hospital names started with the Ascension brand followed by the local name already in place for the recognition of their unique histories within their respective communities. Besides, all facilities adopted the same visual marking, colors, and fonts of the new Ascension logo to unify the sites as one big family of brands.
Rebranding is a long and costly process but it turned out to be worth it as the system’s brand became identifiable and helps employees feel like they are truly part of Ascension. That journey wasn’t a quick one for Ascension which took the company around three years. While it might be tempting to speed through a tedious process, taking your time is important because it’s essential to get full internal alignment before you can get to the external piece.
Before anything changed, Ascension spent two years explaining the rebranding process to its health system’s associates. As most of the associates are very local and very sensitive about their own brands, there’s a need to overcommunicate. The final decision to rebrand came after the time of planning and discussion about the why and the how.
Take Advantage of the Ongoing Digital Transformation
As we all know, the healthcare environment is changing rapidly, largely based on the evolving needs and expectations of our patients and caregivers. Artificial intelligence and big data are ushering in new ways to integrate care delivery models and manage costs. Numerous health systems are now storing medical records in the cloud to enable patients to access test results online and better connect care.
In Impicciche’s opinion, the problem here is that today’s electronic health record systems don’t talk to each other, which can have consequences for patient care and cause caregiver frustration and burnout. Clinical information is often buried in siloed electronic and paper records. When the information is finally retrieved, it is poorly organized and fragmented. As a result, most clinicians work in an environment where data is incomplete and inaccessible.
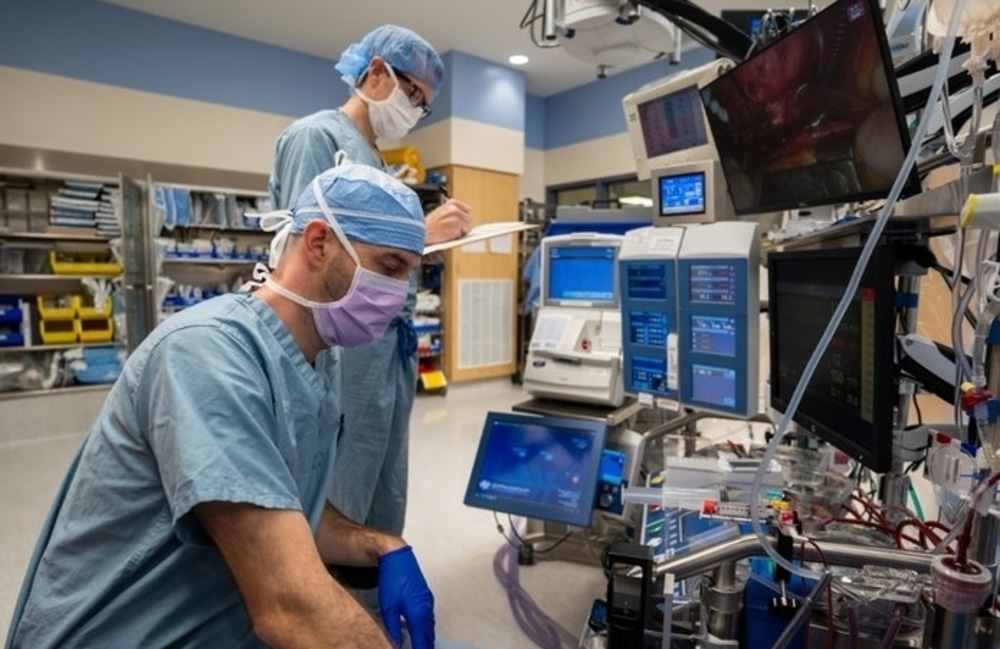
Ascension selected Google to help it on the journey of transformation. Together, they are addressing the interoperability challenges that currently exist with patient medical records to allow for easy, accurate, and secure exchange of patient health information. For security, the health system’s data will always be separate from Google’s consumer data, and it will never be used by Google for purposes such as targeting consumers for advertising.
Obviously, artificial intelligence and machine learning hold promise to support physicians to treat patients more effectively. They help improve care delivery and address well-documented interoperability pain points within the healthcare system. They also help provide insights for licensed clinicians who are always making the final treatment decisions.
Besides the partnership with Google, the healthcare system has launched a number of new programs and products to address technological advancements and customer demands. We can see Ascension Online Care which is a direct-to-consumer virtual care offering available in all 50 states. This platform provides remote access for minor medical issues for patients who need help addressing mental and behavioral health conditions.
“Virtual care expands our portfolio of access points and empowers consumers to choose the best option for their needs,” Impicciche said. “We believe this bold and innovative work will improve clinician experience and patient care in order to save lives.”

End-To-End Revenue Cycle Management Solution Is Key
Hospitals and health systems across the country are facing a revenue cycle management standardization challenge. They all want to address this issue by upgrading their revenue cycle management but the limited capital is often cited as the obstacle because most available capital is invested in clinical technology. This lack of standardization was once the problem at Ascension since it impacted their patient experience.
Besides, sharing services to streamline the revenue cycle can also be difficult as each hospital has its own way of operating. Revenue cycle management vendor partnerships come in a variety of shapes and sizes and that variation becomes challenging as it influences other aspects of care outside of the revenue cycle.
According to Andrew Gwin, Ascension’s Senior Regional Director of Revenue Cycle, the solution was to find an end-to-end revenue cycle management vendor that not only provides a high-quality suite of technology but also acts as a true partner. Such an end-to-end revenue cycle management solution is ideal for standardizing technologies across a large health system like Ascension.
“There are opportunities with end-to-end products, such as reducing your cost to collect, improving your performance, rolling out best practices to improve your normal revenue cycle KPI metrics, and improving the patient experience as well as your technology,” Gwin said.
Indeed, this end-to-end solution provided Ascension with tools for everything from front-end patient access through coding, charge capture, charge reconciliation to back-end functions such as patient financial services, medical billing, and patient collections. It also allowed the health system to standardize revenue cycle management best practices across its hundreds of hospitals.
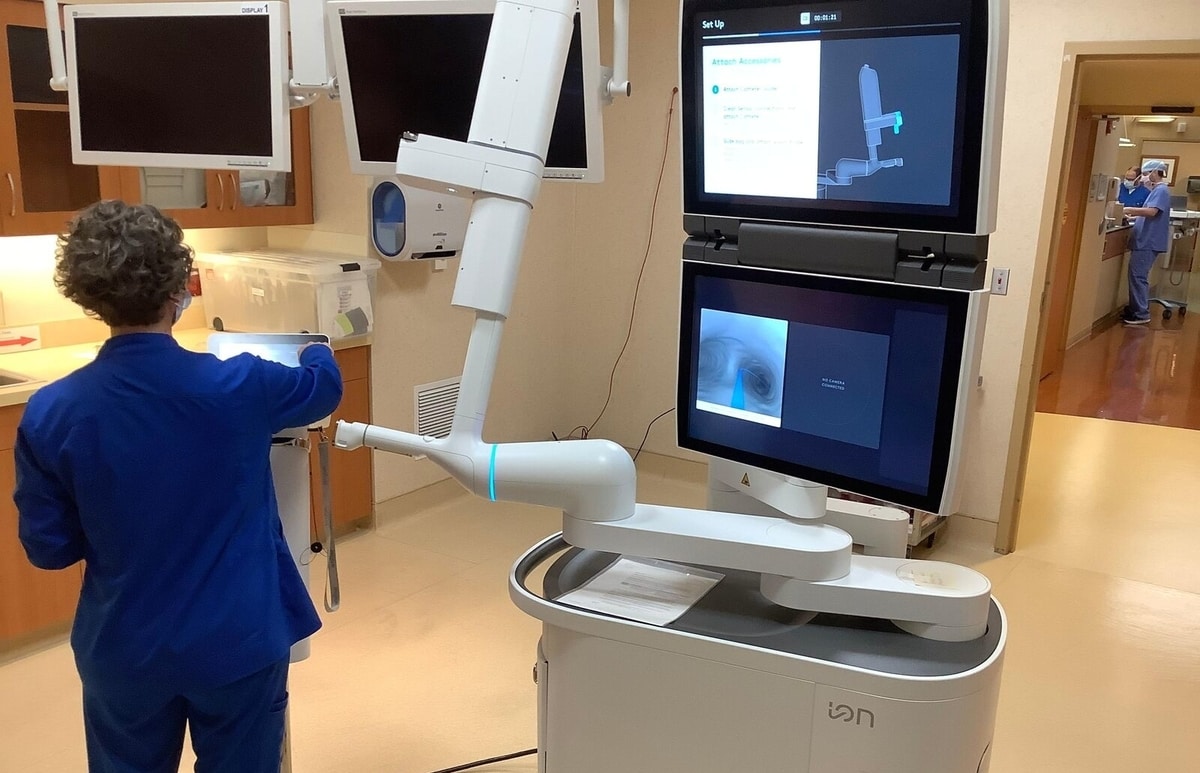
Ascension chose to partner with R1 to implement an end-to-end revenue cycle management strategy and this partnering allows the company to bring the capital to the table in a cost-effective way. “In our case, our contract with R1 works in such a way that we are both incentivized to improve our performance. So, with that improvement, I don’t necessarily have to invest the capital in this partner upfront to receive the technology enhancements that we need to be successful,” Gwin explained.
That practice standardization has actually transformed the hospital-vendor relationship into a true partnership for Ascension since it created not only a standard operating approach but also more specific revenue cycle management best practices. For a solid collaboration, the health system and its vendor have agreed on the best length of the payment plan term.
What we can learn is that end-to-end revenue cycle management solutions are key to improving the business operations of large health systems managing hundreds of hospitals at once. As Gwin said, “It’s technology. It’s best practices. It’s the shared service centers all working together. That’s where you’re really going to drive your ultimate performance and hopefully reduce your costs to collect at the same time.”
The Bottom Lines
From an overall standpoint, we can see that the way to become a leading healthcare system requires a lot of effort and decision-making ability. It’s critical to follow the initial mission on every step and to integrate all associates in the system in the most harmonious way. With that in mind, any healthcare system would achieve even greater results.